The spine, a cornerstone of human anatomy, faces many myths and misconceptions, especially about misalignment. People often think of dramatic vertebrae shifts and believe quick fixes or chiropractic adjustments can easily correct them. However, the truth is much more complicated. Take spondylolisthesis, for example, a real misalignment condition where one vertebra slips over another due to stress fractures. This condition is rarer and harder to fix than many assume. Typically identified in childhood, it complicates the oversimplified views of spinal health, emphasizing the complex relationship between anatomy, injury, and treatment.
Understanding the spine’s blend of resilience and vulnerability is vital before diving into spinal myths. Its ability to recover doesn’t always fit the simple idea of “snapping things back into place.” Sometimes, minimal intervention is enough; other times, surgery is essential to avoid nerve compression. In this blog, we’re set to debunk the myths about spinal misalignment, highlighting the complexities of spinal health and care realities. Let’s explore the scenarios of apparent spinal misalignment together.
Spondylolisthesis
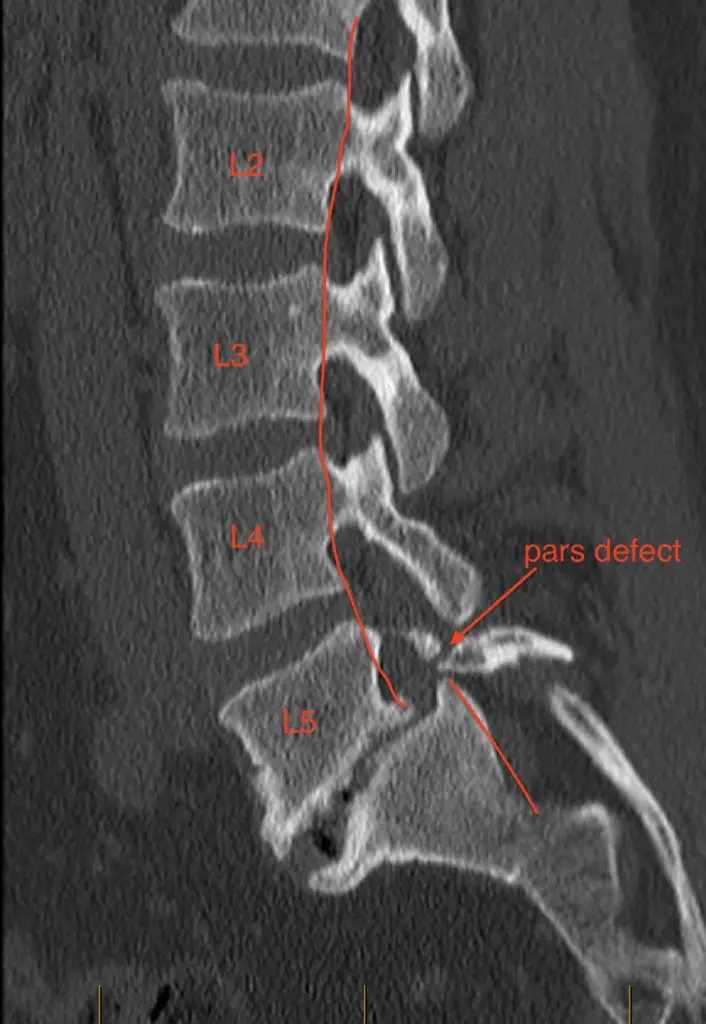
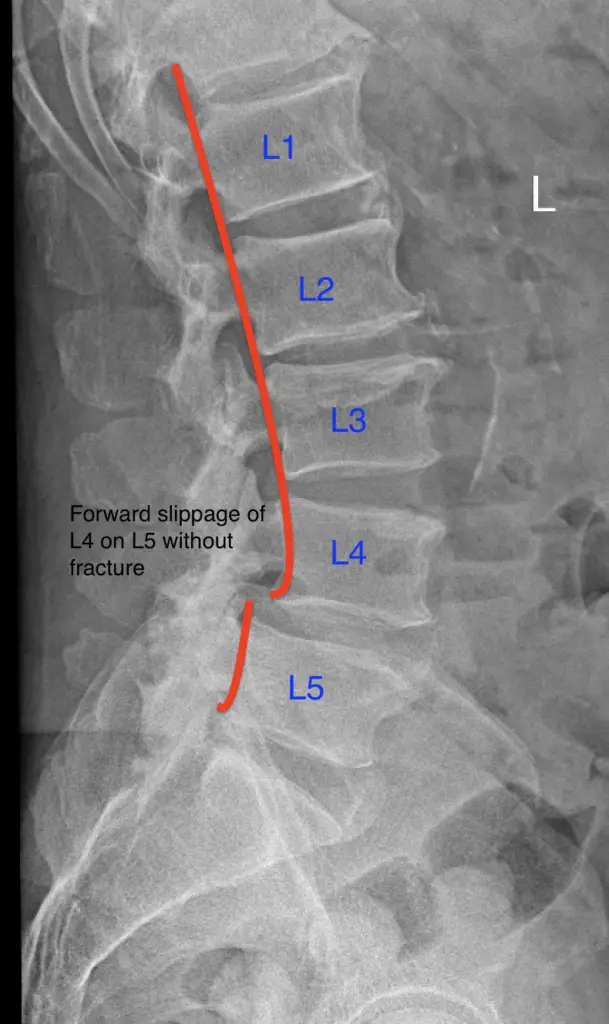
Spondylolisthesis occurs when one of the spine’s bones slips forward over the one below it, similar to a block sliding out of place in a stack. Imagine your spine as such a stack, where each block represents a bone in your spine. This slipping can be due to a small crack or stress in the bone, often caused by injury or overuse. However, not every slip requires medical intervention. Doctors might help if the slip causes pain or puts pressure on nerves.
We also encounter “pars defects,” which further explain spondylolisthesis. Imagine your spine as a structure made of Lego blocks, connected on each side by bridges called the “pars interarticularis.” A crack or break in these bridges, known as a pars defect, can cause a bone in the spine to slip forward, leading to spondylolisthesis.
Various factors can cause pars defects, but they usually result from stress on the spine. This stress can come from activities that involve a lot of bending and twisting, like gymnastics or football, from an injury, or it might be a condition present from birth. Pars defects and spondylolisthesis are more commonly found in active children and teenagers who engage in sports that significantly strain their lower backs.
Degenerative Spondylolisthesis
Degenerative spondylolisthesis is when one vertebra in the spine slips forward over the one below it, not due to a stress fracture but because of the wear and tear accompanying aging. This degeneration can weaken the joints and ligaments that keep the spine aligned, leading to slippage.
Specifically, it often affects the ligaments and capsules surrounding the vertebrae, stretching them beyond their normal limits and compromising the spine’s stability in that area.
Unlike spondylolisthesis, which arises from a stress fracture (often seen in younger individuals and athletes), degenerative spondylolisthesis cannot be “pushed back into place” through manual adjustments or exercises. The underlying issue is not just the position of the bones but the condition of the deteriorated ligaments and joints.
Trauma

If spinal joints are dislocated due to severe accidents or trauma, immediate medical attention in a hospital is crucial. Such injuries, which are beyond the scope of chiropractic care, can cause significant tissue, nerve, and possibly spinal cord damage.
Emergency care, possibly surgery, and rehabilitation are essential for treatment. Specialists aim to minimize pain and restore function, emphasizing the importance of prompt, professional care to prevent further injury and ensure the best recovery outcome.
Acute Disc Injury
When a disc is injured, it may lead to disc herniation, which can result in inflammation and pain in the area. In response to this pain, your body automatically tries to find a position that minimizes discomfort. This response is known as antalgic posture or antalgia. It’s a protective mechanism where your body adjusts its posture to relieve pressure from the injured disc. For example, if the wounded disc is on the left side of your spine, you might lean to your right side to reduce pressure and pain on the left side.
This leaning or shift in posture can give the impression that a bone in your spine has become misaligned. Observers might think that the spine itself has structurally shifted. However, this is not the case. The apparent misalignment is due to the body’s temporary adjustment in posture to reduce pain and pressure on the injured disc.
Subluxations
Chiropractors frequently discuss spinal misalignments or subluxations as a critical reason for pain and discomfort, suggesting that bones can shift out of their proper alignment. However, the concept of bones moving out of alignment is misleading. The human spine is a robust structure designed to support and move harmoniously with the body.
When chiropractors refer to “misalignments” or demonstrate what they claim to be misalignments on an X-ray, it’s crucial to understand that these images might not show a change before and after treatment. What is often perceived or labelled as misalignment might not involve the bones themselves moving out of place in the everyday sense.
Instead, chiropractors often detect and address areas of stiffness, muscle tension, and reduced mobility within the spine. These symptoms can cause discomfort and limit movement, creating the sensation that something is “out of place.”
The Benefits of Spinal Adjustments
Chiropractic adjustments, a core component of chiropractic care, are often misunderstood as a method to correct spinal “misalignments.”
However, their primary goal is not to mechanically realign bones but to enhance joint mobility and improve neurological feedback between the joints and the brain. This clarification helps to demystify how chiropractic adjustments contribute to improved health and well-being.
Sedentary postures and excessive computer and phone use can create tension in the muscles surrounding joint structures. Chiropractic adjustments address these issues by applying controlled forces to joints that have become restricted in movement. They can increase the range of motion, reduce pain, and improve joint movement efficiency.
The enhanced mobility following an adjustment can also lead to better neurological feedback. Each joint in the body is surrounded by nerve endings that send information about movement and position to the brain. Therefore, improving joint function can enhance the brain’s ability to perceive how and where the body moves in space, known as proprioception.
This enhanced feedback loop helps the body maintain balance, coordination, and overall physical function.
Conclusion
In exploring spinal health, we debunked myths about spinal misalignments and clarified the roles of chiropractic care and conditions like spondylolisthesis. We learned that the spine is a complex structure, and care often involves improving joint mobility and addressing lifestyle factors such as sedentary behaviour and phone use. For conditions like degenerative spondylolisthesis, treatment varies, with surgery as an option for severe cases, though not commonly needed.
Understanding and managing spinal health requires a multifaceted approach, blending medical insight with lifestyle adjustments. This discussion highlights the importance of informed choices in spinal care, aiming to enhance well-being and prevent spinal issues effectively.

